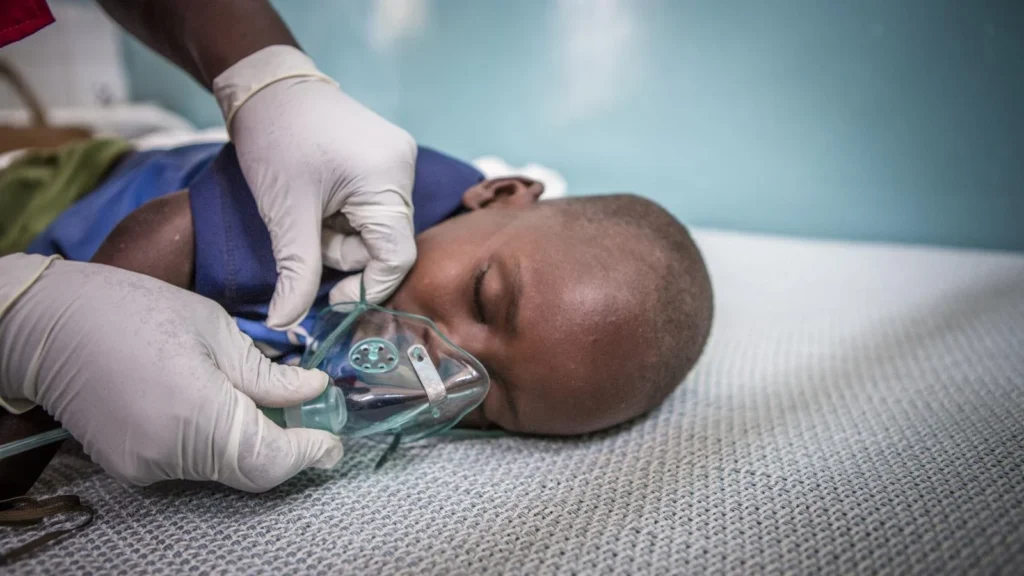
The precarious nature of labor in Kenya is starkly illustrated by the daily realities of motorcycle taxi operators, locally known as “boda-bodas,” who frequently endure hazardous working conditions for wages averaging just $1 per day. Patrick Maina, a former operator who suffered a debilitating spinal fracture in 2021, exemplifies the profound systemic failures of the region’s healthcare infrastructure. Despite possessing the physiological potential to walk again, the prohibitive costs associated with essential physiotherapy and ongoing medical interventions remain an insurmountable barrier for Maina and millions like him.
Macroeconomic Pressures and the Imposition of Austerity
This localized tragedy is inextricably linked to broader macroeconomic forces and international financial governance. Kenya, mirroring the fiscal realities of numerous African nations, is currently classified as being in “debt distress” by the International Monetary Fund (IMF). This precarious financial status grants the IMF and the World Bank—collectively known as the Bretton Woods institutions—extraordinary leverage to dictate domestic public policy. Historically and presently, these organizations advocate for stringent neoliberal economic frameworks, mandating severe austerity measures that disproportionately impact the working class. While these institutions generally refrain from explicitly demanding reductions in healthcare budgets, the decimation of public health funding is the inevitable corollary of loan conditionalities that mandate public sector contraction and the widespread privatization of state assets to prioritize foreign debt servicing.
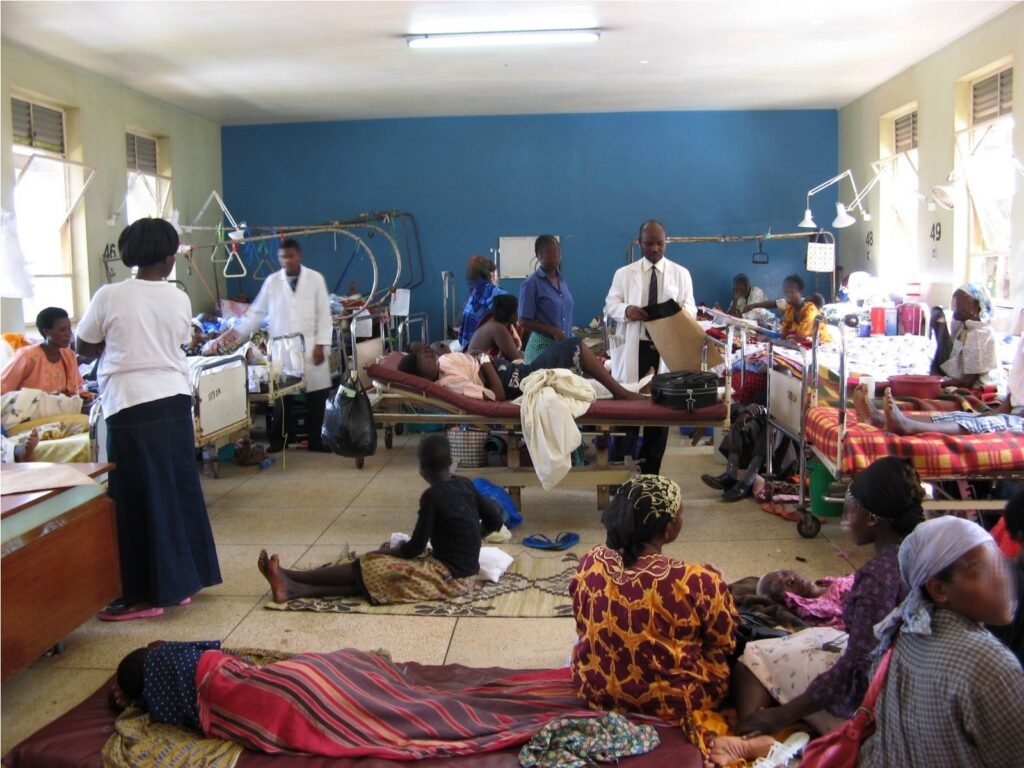
Ultimately, these structural interventions have largely failed to stimulate sustainable economic growth, instead entrenching cycles of debt and systemic poverty.
The Illusion of Universal Coverage in Kenya
In response to these fiscal pressures, Kenyan President William Ruto recently implemented healthcare reforms ostensibly designed to establish a framework for universal health coverage. However, the resulting “Social Health Authority” (SHA) operates as a highly regressive system. The SHA mandates financial contributions from all citizens, encompassing those earning sub-poverty wages and incapacitated individuals entirely unable to participate in the labor force.
From a macroeconomic standpoint, this broad taxation functions as a mechanism to consolidate state revenues, thereby satisfying IMF requirements to expedite sovereign debt repayments to Western creditors. Consequently, highly vulnerable individuals are coerced into financing a system from which they are effectively excluded. Maina, despite being unable to work for years, is required to pay monthly premiums of 500 Kenyan Shillings (approximately $4) without receiving any reciprocal medical assistance or coverage from the SHA. Concurrently, public hospitals remain chronically underfunded and underequipped, driving desperate patients toward prohibitively expensive private facilities. Reports indicate that some of these private institutions are so costly that their own medical staff cannot afford treatment there.

The Historical Roots of Healthcare Divestment
The contemporary healthcare crisis is the culmination of decades of structurally imposed austerity. Economic historians trace this trajectory to the early 1980s. Throughout the 1970s, Western financial institutions aggressively promoted borrowing to African nations to capitalize on historically low interest rates. However, the 1983 “Volcker Shock,” wherein the US Federal Reserve abruptly and unilaterally raised interest rates, triggered an immediate and devastating continental debt crisis.
The Bretton Woods institutions exploited this newly acquired leverage to mandate severe structural adjustment programs, leading to catastrophic divestment from public healthcare systems. Professor Howard Stein of the University of Michigan notes that between 1976 and the late 1990s, per capita health expenditure plummeted across the continent; Ghana’s spending dropped from $10 to $6, Zambia’s from $14 to $11, and Nigeria’s from nearly $3 to $1.81. The imposition of neoliberal user fees in Kenyan clinics coincided disastrously with the accelerating HIV pandemic, contributing to a severe decline in regional life expectancy from fifty to forty-six years between 1980 and 2002.
Despite mounting public pressure that forced the creation of the Highly Indebted Poor Countries (HIPC) Initiative in the late 1990s, the conditionalities attached to this debt relief merely entrenched neoliberal policies further. Empirical research by Alexandros Kentikelenis and Thomas Stubbs demonstrates that IMF conditionality continues to drive healthcare privatization and the price liberalization of basic goods, resulting in demonstrably negative public health outcomes regardless of overall government expenditur e levels. These policies negatively correlated with vital indicators such as maternal and under-five mortality, vaccination coverage, and health worker density, only inadvertently improving public health by rendering tobacco products too heavily taxed for daily consumption.
The Cruelty of Commodified Care and Pcatient Detention
The human toll of this aggressively commodified system is severe. Following his accident, Maina required urgent spinal surgery, but under-resourced public facilities necessitated his transfer to a private hospital. While patients in fully developed healthcare systems would typically receive such surgery within 24 hours, Maina languished for three weeks. His family was forced to liquidate essential assets—including selling livestock and his motorcycle—and solicit community donations merely to secure the initial surgical deposit. Following the procedure, the hospital detained him for an additional six months until his family could source the remaining balance.

This practice of medical detention is alarmingly normalized. In another tragic instance, Mater Hospital in Nairobi detained the deceased body of Caroline Tito for nearly two months over an unpaid bill exceeding $25,000, requiring High Court intervention to force the release of her remains to her orphaned sons. An Oxfam report highlighted similar systemic abuses at Nairobi Women’s Hospital, an institution notably funded by the World Bank’s private-sector arm, the International Finance Corporation (IFC). The hospital has reportedly imprisoned patients, including newborns, for months over unpaid invoices. Linda Oduor-Noah of Oxfam International notes that in IFC-backed facilities, the profit motive supersedes patient welfare, leading to egregious human rights violations, price rigging, unnecessary treatments, and the denial of emergency care.
A Continent-Wide Crisis
This paradigm of exclusionary, for-profit healthcare extends across the African continent. In Morocco, World Bank investments have prioritized private oncology centers that exclusively serve the salaried middle class, exacerbating public dissatisfaction that culminated in recent protests demanding public hospitals over state infrastructure projects. In Nigeria, IFC-funded facilities such as Hygeia’s Lagoon hospitals charge maternity fees equivalent to nine months’ income for the poorest half of the population.
Rather than fortifying public health systems to meet overwhelming societal demand, international finance institutions continue to channel critical resources into inaccessible private enterprises. Despite Oxfam’s 2023 Sick Development report demanding an immediate cessation of direct and indirect public funding for for-profit healthcare, institutions like the World Bank remain intransigent. They continue to ignore compounding evidence of the severe harm their investment strategies inflict on the continent’s most vulnerable populations, leaving millions of citizens like Patrick Maina structurally abandoned.